This article is taken from Innovations in Pharmaceutical Technology, April 2019, pages 15-17. © Samedan Ltd
Geoff Gill MS at Shimmer
Wearable sensors provide realworld data that can potentially create new endpoints which reduce the size and shorten the duration of clinical trials. The FDA is very supportive, with Commissioner Dr Scott Gottlieb stating that leveraging real-world data to improve regulatory decisions is a key strategic priority for the Agency (1). The FDA also introduced a new strategic framework to advance use of real-world evidence to support development of drugs and biologics in December 2018 (1). According to the Clinical Trials Transformation Initiative, “Mobile technologies for data collection [including wearable sensors] should be considered in all future trials to improve the quality and efficiency of clinical trials and the value of the data they collect.” (2)
Integrating a new technology into an already complex and expensive clinical trials process can be daunting. The pharmaceutical industry has little experience in using wearable sensors in the
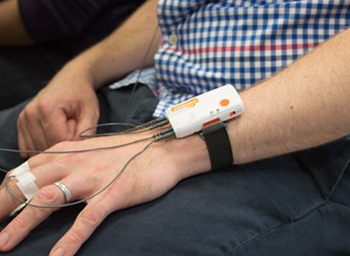
field at any kind of scale. The industry needs to figure out how to introduce these technologies at minimum cost and potential for failure. Consumer wearables may provide value in some cases, but they were designed for a completely different purpose: to provide easy to- understand, but not necessarily scientific, metrics for their users. [Shimmer NeuroLynQ Sensor below]
Their shortcomings for clinical trials include the inability to provide raw data, lack of algorithm validation and transparency, and inflexibility in the types of data they collect. These shortcomings will significantly limit the viability of consumer wearables for clinical trials.
However, the pharma industry can learn from the consumer neuroscience field, which uses tools created for neuroscience to better understand consumers. Companies in this industry have monitored millions of study participants at relatively low cost. For example, working with partners, Innerscope Research developed a kiosk infrastructure that allowed it to collect medical grade electrocardiograph (ECG) and galvanic skin response data from hundreds of participants in a single weekend across several cities, at a total cost of less than US $50 per participant. In many cases, accuracy requirements for a consumer neuroscience study surpass even medical requirements. For example, consumer neuroscience analysis requires that the sensor reliably detects every single heartbeat. Averages over time or sample ECG waves are inadequate. The following six lessons from consumer neuroscience should be applied when implementing wearables in clinical trials.
Make It Easy for Participants
Trial participants are asked to do a lot. The more complex you make the process, the lower the compliance will be. Using the wearable sensor needs to be as simple as possible for participants and also needs to be foolproof, otherwise, people will make mistakes that you would never consider. For example, in a recent demonstration of consumer neuroscience technology to a sophisticated group of market researchers, a number of them did not remove the plastic backing from disposable adhesive electrodes, taping the electrodes to their skin with medical tape. These were very smart people who just had no experience with this particular technology. Remember, what seems obvious to you may not be to someone with no background in the subject. Ideally, he participant should not have to do anything but put the wearable on once and leave it there for the entire trial.
Collect Raw Data and Build a Database
Access to the raw sensor data is vital for many reasons. Examining the raw data may help you understand and even address anomalies in the data. If a participant puts their sensor into the dryer by mistake or onto their dog for some reason, you may get a very distorted number of steps. With the raw data, the different movement signatures would be
very clear, and it would be easy to justify removing those points from the database. Without access to the raw data, it may be difficult or impossible to resolve the issue. Raw data also enables tailored metrics to be developed. For instance, a wrist-based inertial measurement sensor could be used to measure Parkinson’s tremors or count the number of times someone goes to the bathroom at night, but only if you capture the raw data. With this, a database can be built that has value over multiple studies and devices. The raw data will be comparable across many or all the devices that can be used. Over the past 10 years, thousands of researchers around the world have been developing and validating algorithms to measure innumerable metrics of interest, all based on raw data. An algorithm validated based on raw data from one device can easily be transferred to other devices producing the same raw data. The alternative is validating the metrics from each device from the ground up. Furthermore, a database of raw data not only allows you to develop norms, but may also provide the data to test and validate new algorithms that are developed over time. The further away from raw data you get, the more difficult it will be to validate and transfer it.
Keep it Simple: Measure What You Need
In many cases, studies will not need the standard medical data, and it will be possible to greatly simplify data collection by collecting something different. As previously mentioned, consumer neuroscience requires extremely reliable capture of every beat-to-beat interval with an ECG. However, it does not need the morphology of the waveform at all. Because of this, it was possible to greatly simplify the data collection process by putting electrodes on opposite wrists, eliminating the need for participants to remove their shirts. By clearly understanding the output required, the overall data collection process could be made much simpler.
Real-Time Study Management Tools are Vital
There are always surprises in the course of implementing studies. Unexpected gaps in data capture may emerge, and different sites may have different results. By quickly identifying and addressing these issues, the trial managers may be able to avoid large or even disastrous issues later. This requires a system that allows you to monitor what is going on and easily identify issues as they emerge. In Innerscope’s kiosk example mentioned earlier, every site’s recruiting results were available in near real time. If certain sites were having trouble meeting their recruiting goals for a particular demographic, the study manager could dynamically reallocate quotas to different sites to keep the project on track. When collecting wearable sensor data remotely, it will be important to know from the beginning that you are getting the data you need. If one site is having particular trouble achieving compliance, you need to be able to identify that and correct it quickly. If all sites are having trouble, protocols may need to be changed. In any case, the sooner the issues are identified, the more likely you will be able to recover from them.
Pilot Data Collection Techniques on Employees
Testing your protocols by running pilots is vitally important. It may seem obvious but, in the rush of trying to get a trial off the ground, companies may skip this step. In almost every case, that will be a mistake, as something unexpected will happen in the data collection. However, the time pressure once a study is moving forward is real. For that reason, it is important to start testing devices ahead of time – even before a study starts. Consumer neuroscience companies almost always use their employees as beta testers for a data collection technique. If you cannot get employees to wear a sensor and collect data successfully, asking a participant to do it is probably unrealistic. Not every failure will be caught with this approach, but many will appear and be correctable.
Leverage Partners
The consumer neuroscience systems discussed were all built with close cooperation between multiple partners. Implementing wearables in a clinical trial requires pharma companies to enter realms where they have far less experience. To make this transition effectively, they will need to rely on partners who will work with them to meet the unique requirements of their clinical trials. Obviously, device companies will be important
in this collaboration. The ability and willingness of a manufacturer to collaborate and be open with their technology and algorithms should be a critical criterion when choosing a wearable device. Beyond the device manufacturer, pharma companies should look to partner with each other. Achieving the true potential of wearables in improving clinical trials requires developing validated outcome measures in numerous different therapeutic areas. However, this work is truly precompetitive. Having accepted outcome measures will benefit all pharma companies, and there is no real advantage to developing proprietary outcome measures. For this reason, the industry should collaborate and work together in this process.
The Sensor Future
Using wearable sensors in clinical trials has the potential to address one of the most challenging problems in the pharma industry today: reducing the spiralling costs of bringing a drug to market. Six lessons have been identified from the consumer neuroscience industry to help make this a reality. However, in the end, the most important message is the need for transparency and collaboration across the pharma industry, wearable sensor manufacturers, and academia. Achieving wearables’ potential to improve clinical trials is a large task, which will be accomplished much more easily and faster if we all work together in a precompetitive fashion.
References
1. Visit: www.fda.gov/NewsEvents/ Newsroom/PressAnnouncements/ ucm627760.htm
2. Visit: www.ctti-clinicaltrials. org/sites/www.ctti-clinicaltrials. org/files/mobile-technologiesexecutive- summary.pdf